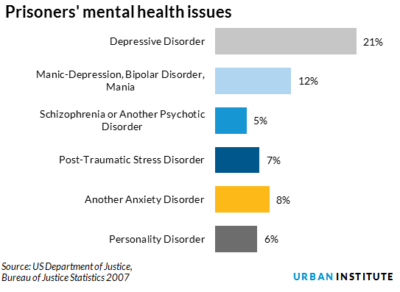
This post is about a prison memoir, BLOOD ON THE RAZOR WIRE, not mental illness.
(5-8-23) Chad Marks turned his life around by sheer determination and guts.
Raised by a single mother on welfare in a poor Rochester neighborhood, he started selling cocaine when he was thirteen years old. Three years later, he was selling crack cocaine and when he was 24 years-old, he was sentenced to a 40-year federal mandatory minimum sentence – ten years for a crack cocaine drug conspiracy, five years for possessing a weapon, and another 25 years for possession of a .22 rifle.
Society was happy to rid itself of him. And it did.
Marks was sent to “Big Sandy,” a federal maximum security prison located in a remote area of Kentucky. It was one of the most violent penitentiaries operated by the federal government, with stabbings, beatings and murders.
Chad Marks was not prepared for what he was being thrown into as a young man facing four decades behind bars.
“For me there was a choice I had to make,” he later would write in an article for Families Against Mandatory Minimums. “I could give up, and in doing so take a road of negativity, or I could choose a much different path. I saw then that all paths in life, for good or bad, begin with one small step. For so long in my life, I chose the wrong path. At that very moment, I knew I had to change my direction, because when we choose our path we choose our destination.”